
17 Sep Interventions for sensory issues in children
“Raj, learn to keep your eyes open when you walk!”
“Sweety, it’s just the washing machine. Don’t be scared.”
“John, why don’t you finish your apples, it’s exactly what you like eating every day.”
The above statements might remind you of how your day typically is with your child. As a parent, it’s frustrating to know, how your child can be upset/have a meltdown about such small things. Does it feel that you are raising a fussy child? or your child is being unimaginably difficult? The answer is “No” The answer to understand your child’s such concerns is knowing the sensory processing challenges your child goes through. https://littlepods.in/introduction-to-sensory-processing-disorder/
The primary plan to manage the child’s sensory integration issues begins with a consultation with an expert who has specialized in the area of sensory integration most often an Occupational Therapist. The sensory integration approach to occupational therapy at is best used to treat SPD; the goal of intervention is to enable a child’s nervous system to more efficiently process and respond to sensory information. Additionally, a counselling plan and a parent management training may include systematic desensitization-children increasing coping with uncomfortable stimuli through increased exposure to equip them to deal with the sensory challenges in the day to day life.
The purpose of the intervention team is to collaborate on the child’s needs and work across various settings. It comprises a school counselor/ psychologist (e.g., school counselor, mental health counselor), Occupational Therapist, Parents/caregivers, and Teachers. The intervention team may include the child’s paediatrician and potentially a nutritionist when appropriate. Counselors can play a vital role as part of a treatment team by coordinating the interdisciplinary team. Also, family involvement is crucial-parents or caretakers often know their child best on a long-term basis. Early SPD diagnosis and treatment is crucial in assisting children with SPD symptoms (Ben-Sasson et al., 2009; Byrne, 2009; Miller, 2006). SPD diagnosis and treatment early in life has a quintessential impact on a child’s developing brain and behavioral symptoms.
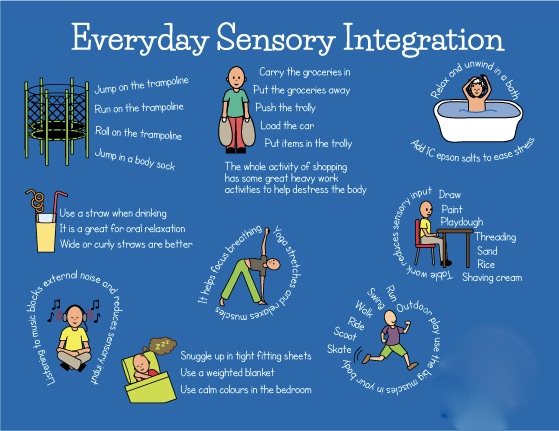
Some tips on Managing Sensory Processing Disorder according to specific concerns:
Those with higher sensitivity in vision; changes in the environment such as reducing fluorescent lighting (photosensitivity), providing sunglasses, using blackout curtains, creating a workstation in the classroom – a space or desk with high walls or divides on both sides to block out visual distractions has been found to be helpful. Children with hypo-visual sensory needs providing visual supports or coloured lenses are recommended, but there is limited research for lenses.
Those with hypo-auditory (sound) sensitivity using visual supports includes colored picture, photographs, symbols, or written words to back up verbal information, and ensuring that other people are aware of the under-sensitivity. Managing hyper-auditory (sound) sensory concerns in a child by using earplugs, shutting the doors or windows to avoid loud noise, preparing them before entering loud noise area (during an annual day in the school, birthday parties, and so on). Showing videos or being in the same set u a day prior to the event, or even making the child visually aware of what the place looks and sounds like are some additional helpful strategies.
By providing strong-smelling products like mild perfumes, body mists, scented oils to distract from inappropriate smell or meltdowns associated to hyper olfactory sensitivities (smell) can be helpful to manage with hypo-gustatory/hypo-olfactory sensory sensitivity. Managing children with hyper-olfactory issues can include avoiding the use of unscented detergents or shampoos, avoid wearing perfume, and making the environment as fragrance-free as possible.
Children with hyper-tactile sensory needs can be treated by giving different textures of food or slowly introducing different textures around the person’s mouth, such as a flannel, a toothbrush and some different foods. Remedies for hypo- tactility (oral sensory) may include latex-free tubes (for chewing), straws or hard sweets (chill in the fridge). Games like Treasure Hunt – hiding small objects in play Doh or to a tactile box to find with fingers. Painting outdoor with water, paint roller in bathtub, soap crayons or drawing in sand or salt; using therapeutic putty.
Dealing with vestibular hyposensitivity may include rocking horses, swings, and roundabouts, seesaws, catching a ball or practising walking smoothly up steps or edges. Breaking down activities into small, more easily manageable steps and using visual cues such as a finish line, to balance their body providing appropriate chair and table so that they can sit upright this will help to deal with children who have vestibular hypersensitivity.
Using weighted blankets to provide deep pressure, firstly is often helpful to calm your child. Secondly, the use of colored tape on the floor to indicate boundaries. Making the child aware of the distance from others by using the ‘arm’s-length rule’ to judge personal space – this means standing an arm’s length away from other people (use of hula-hop, color tape, and so on). These remedies might help to train the children with proprioceptive hyposensitivity. Proprioceptive hypersensitivity can be deal by giving fine motor skill activities like beads (beginning with bigger one and later decreasing the size), lacing board, and picking softballs by using a clothespin, visual scanning pencil control activities like mazes, find the differences and so on.
These interventions can be used during therapy sessions or at home under the guidance of a counselor or occupational therapist. The ideal plan of action for a child with sensory processing issues is also when the child gets used to doing such activities at home as fun even with family and parents This will benefit developing the interpersonal relationship. Adjusting to the environment and perceive and process environmental stimuli. Help to develop positive behaviour pattern and eliminate fear in every environment. It is of the utmost priority that parents as therapists get trained to work with the child’s sensory needs at home under close guidance and supervision of the Occupational therapist or an expert, as it is known that any environment or even in the home set up the child could feel overwhelmed and have a meltdown, hence the right approach is on learning to work through the triggers rather than completely shield the child.
Let us help your child with sensory processing issues do better in school!
A remarkably well-known fact related to the treatment of sensory processing; lies in an occupational therapy based approach where the child should be engaged in some physical activities that are designed to regulate the child’s sensory input. These approaches can be also adapted to an inclusive set up like the school and classroom, where just a few practical changes in the child’s set up and schedule can make him/her enjoy the school hours making the whole experience more productive. Classroom-based interventions can not only help the teacher and school team but also makes the child feel more comfortable, secure and focused in the classroom.
Some workable interventions at school are:
- Some kids are better off if they sit close to the teacher. However, if your child is easily distracted by noise, he may end up turning around often to where the noise is coming from.
- Make sure his/ her seating arrangement/ chair is a good fit for him. When the child is sitting at his desk, he should be able to put his feet flat on the floor and rest his elbows on the desk.
- Make sure he’s not sitting next to distracting sources of noise.
- For the child who needs to move a bit, you might try an inflated seat/ cushion or a pillow from home, chair with rocky wheels so he can both squirm and stay in his seat depending on his /her specific need.
- If possible, eliminate buzzing and flickering fluorescent lighting to provide consistent visual sensory support.
- The Occupational Therapist can also work with the child on knowing where his/her body is in relation to other people and things and the idea of personal space, pressure and distance we maintain while we play/speak.
- It is of utmost importance to understand and provide sensory breaks to the child such as walking in circles, jumping on a mini-trampoline and sucking on sour candy so he gets the input he craves and doesn’t bump into others. These breaks need to be well planned and executed to avoid meltdowns.
- Allow for fidgets and chewable items, available in OT catalogues, to provide input
- Both gross and fine motor skills need to be consistently worked with the child to boost a sense of self-confidence and let the child perform different activities.
- Allowing the child to skip school assemblies, or sit near a door so that he can take breaks in the hallway with a teacher when he starts to feel himself getting overwhelmed are good ways of avoiding meltdowns and bolting, however, they have to be well monitored as the child can also pick up escape behaviors from such breaks.
- Sometimes the cafeteria or the school canteen may be too stimulating, The child can be initially made to sit with one or more lunch buddies eat in a quieter room with a teacher or shadow support, gradually sensitizing him to a bigger space like the cafeteria.
- Have a clear visual schedule posted with plenty of preparation for transitions and also letting the child know about his/her scope of asking for a break. Planning and preparing ahead of any changes or transitions can help the child focus and cooperate better.
Through the help of such daily workable interventions and with the cooperation of parents and school, a child with sensory processing issues can be made to well adjust to the school experience as well as we can prime them for success.
Let’s challenge ourselves to understand and provide the necessary assistance to children with sensory concerns in the best empathetic sense!!



No Comments